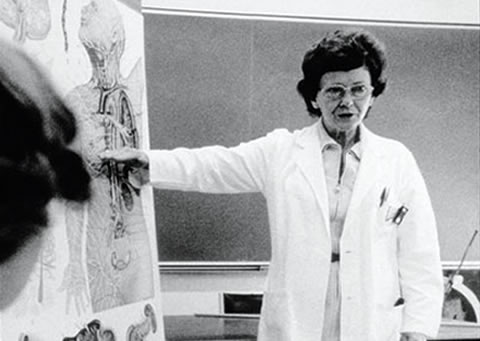
Open U of T’s 1934 yearbook, and you’ll find photos of 115 graduating medical students – only 10 of whom are women. Among them is (Mildred) Vera Peters, who went on to revolutionize how Hodgkin’s lymphoma and breast cancer are treated.
As a radiation oncologist at Toronto General Hospital, Dr. Peters learned that many patients wouldn’t go to the doctor if they suspected they had cancer. In the 1930s, being diagnosed with Hodgkin’s was like being handed a death sentence. By 1950, though, Peters and colleagues had determined that high-dose radiation could cure this lymphatic cancer if caught early. She began a lifetime crusade to encourage patients to seek prompt treatment and overcome what she coined “cancer phobia.”
Women who found a breast lump were also afraid to seek medical attention: the standard treatment for breast cancer was a radical mastectomy, in which the surgeon removed the entire breast. But with early-stage breast cancer, Peters excised only the tumour. In the mid-1970s, Peters, who was a professor of radiotherapy and medical biophysics at U of T, published a retrospective study of the 8,000 breast cancer patients she had treated. It showed that treating the cancer in its early stage with a lumpectomy and radiation produced the same survival rate as a radical mastectomy.
“I was refuted and shunned by most of the outstanding surgeons in the States,” Peters told the Oakville Medical Society in the early 1980s. She remained steadfast and as more studies found the same results, she optimistically wrote, “Mastectomy in early breast cancer may become as old-fashioned as bloodletting.”
Recent Posts
U of T’s 197th Birthday Quiz
Test your knowledge of all things U of T in honour of the university’s 197th anniversary on March 15!
Are Cold Plunges Good for You?
Research suggests they are, in three ways
Work Has Changed. So Have the Qualities of Good Leadership
Rapid shifts in everything from technology to employee expectations are pressuring leaders to constantly adapt