In cities across Canada, homeless people bounce from street to shelter. They rarely visit doctors, except in emergencies, and untreated mental illness, addiction, malnourishment and serious chronic health problems are common. Now, a U of T-led study is suggesting a new approach to helping the homeless. The At Home/Chez Soi study shows that providing apartments to people who are homeless and living with serious mental illness costs about the same as the usual referrals to shelters and crisis care, but yields significant improvements in quality of life.
Led by psychiatry professor Paula Goering, the federally funded study enrolled 2,256 homeless people with serious mental illness, starting in 2011. Half the participants were randomly assigned to receive housing, while the others received the usual referrals.
Those who received housing were taken to view apartments in their preferred neighbourhood; the client’s choice was rented. At Home supplied furniture. There were only two conditions to the housing offer: participants would contribute 30 per cent of any monthly income toward the rent (At Home subsidies provide the remainder), and they would agree to a weekly visit from a case manager. “We weren’t enforcing that people accept treatment,” Goering explains. “It was just so we could monitor what was happening.”
What happened was intriguing. “Almost universally, people start asking for help,” says Goering. “They want to keep their place: the stability, privacy and safety.” And because clients were now seeking help before reaching a crisis point, they could receive more preventive and primary care – a better use of public resources than 24-hour or emergency services.
Rose Harrison is one of the participants who received housing. In late 2010, battling untreated bipolar disorder and schizophrenia, and racked with grief over the death of her 16-year-old son from leukemia, she huddled over vents, waiting for dawn, terrified for her safety. The following March, social agencies connected her with At Home.
Since getting the keys to her own apartment at Yonge and Eglinton, Harrison, 43, regularly sees a doctor, who stabilized her medication regime. She receives disability payments, and – she breaks into a smile – “I work, at the LCBO. I clean that whole store; I work three hours a day. And I am so content with that.”
“‘Housing first’ is the study’s tagline,” says Goering, “but it’s not housing only. It’s housing first, then support – support that honours the individual’s choices, provides a whole range of different resources. That’s very important.”
Goering and her research team, which includes U of T professors Stephen Hwang, Vicky Stergiopoulos and Patricia O’Campo, are still analyzing data for their final reports this December. But they know that the savings in health care and homeless shelter costs for participants nearly offset the program’s costs. While health outcomes improved equally in both groups in the first year, At Home participants are getting preventive care that may show better results in the long term.
In March, the federal government announced five-year annualized funding for an approach across Canada that’s similar to what’s used by At Home. Municipal agencies in any city can apply – and people already enrolled, such as Harrison, will be able to keep their homes. “Being homeless is the worst,” says Harrison. “I pray for every homeless person to have the opportunity that I have to be able to turn my life around and to be independent – to control my own money and my life.”
Recent Posts
People Worry That AI Will Replace Workers. But It Could Make Some More Productive
These scholars say artificial intelligence could help reduce income inequality
A Sentinel for Global Health
AI is promising a better – and faster – way to monitor the world for emerging medical threats
The Age of Deception
AI is generating a disinformation arms race. The window to stop it may be closing


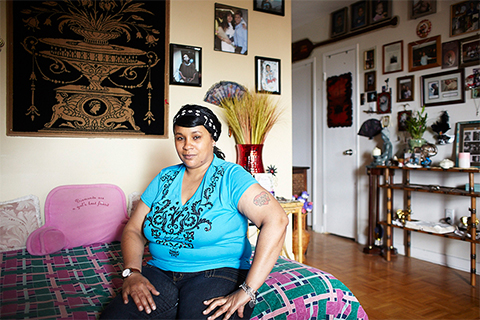


5 Responses to “ Housing First ”
Who were the community partners who did the face-to-face ground work with the people who required counselling and housing assistance?
Why is there no mention of the organizations who partnered in the At Home/Chez Soi study here in Toronto?
This research is not possible without the hard work of faceless, poorly paid, mostly racialized front-line workers who deserved to at least be acknowledged with a reference to their community agency employers. U of T can and should do better!
Dr. Paula Goering responds:
It was an omission on my part not to make sure that credit was given to the community-service providers and to the participants and persons with lived experience who have made the study possible. In Toronto the service agencies included Community Occupational Therapists Associated, Toronto North Support Services, Across Boundaries, Housing Connections and the City of Toronto. A Persons With Lived Experience Caucus also contributed a great deal to the project. In each site there were similar partners who are too numerous to be named. Proper acknowledgements should also include The Centre for Research in Inner City Health and the leadership team from the Mental Health Commission of Canada (Cameron Keller, Catharine Hume and Faye More).
Thank you for this article about a great project. I first read about this concept, with regards to a pilot in an American city, a few years ago in an essay in "What the Dog Saw," by Malcolm Gladwell. At the time I hoped it would spread here. Thank you also for clarifying the people implementing the program here. This must have been a lot of effort, but a feel-good to be able to make such a positive impact in someone's life. I'd love to see a follow-up with longer term results. I hope it continues to show measurable results and that it's worth it on ALL levels to proactively treat people as the worthwhile human beings they are, instead of treating them as if they don't exist, and then reacting to a disaster later.
Thank heaven someone has realized that this is a solvable problem! Mentally ill people wandering the streets make areas less safe not only for themselves but for others, who cannot predict their response to any confrontation, from a complaint to a simple kindly offer of help.
Please make this housing and support program as widespread across Canada as possible, as fast as you can!
What a great project, reading about it really warmed my heart. Well done all involved.