Two hospitals could not seem further apart.
The Hospital for Sick Children in downtown Toronto is a prominent pediatric teaching hospital. Its $320-million annual budget supports a maze of wings that beep and gleam with the ministerings of high-tech health care.
Halfway around the planet in Zimbabwe, at the juncture of two rivers, sits the Salvation Army Howard Hospital, a modest cluster of buildings – some with grass thatched roofs – on grounds made verdant with baobab trees and cheered by the cartoon-bright colours of bougainvillea. With its two physicians and paltry $40,000 annual budget, the Howard serves a population of 250,000 who eke out nourishment and a livelihood from the exhausted soils of the surrounding Chiweshe communal lands that date back to Zimbabwe’s white rule and the segregation of the region’s Shona-speaking people.
Still, the chipatara – Shona for hospital – is a symbol of hope and relief to a people pummelled by hunger, troubled politics and a devastatingly high incidence of HIV infection (one in four Zimbabwean adults have AIDS or are HIV-positive).
It is here that Elizabeth Mufuka, a single mother and subsistence farmer, arrived last June with her belly distended from seven months of pregnancy.
And it is here that Dr. Paul Thistle, who was born in Toronto and educated at the University of Toronto, is the chief medical officer. Alerted by a midwife who suspected the quiet, humble woman was carrying more than one child, Dr. Thistle pulled out the hospital’s most high-tech piece of equipment – an ultrasound – and discovered something troubling. Mufuka was carrying conjoined twins.
Thus began an extraordinary adventure of separateness and togetherness – an effort in which University of Toronto doctors working from opposite sides of the globe pooled resources, resolve and rare surgical expertise so two Zimbabwean babies born with bodies fused together could have a shot at leading separate, healthy lives.
***
“At Howard Hospital, we no longer believe in miracles – we rely upon them,” writes Thistle in Howard Hospital’s 2003 annual report. “It is only by the Grace of God that the hospital remains operational.” Dr. Thistle, a spectacled, youthful 42-year-old, is a revered chiremba – doctor. Since arriving in 1995, the obstetrician and gynecologist is at times the only physician at Howard; on average he sees 150 patients daily. What keeps him in this small village, 80 kilometres and a few bumpy dirt roads north of the capital city of Harare, is an old-fashioned missionary-like dedication. It is also his home. His wife, Pedrinah, is Zimbabwean, and both of their young sons were born at the Howard.
Before Mufuka, Dr. Thistle had seen only one other case of conjoined twins. Attached at the heart and chest wall and born prematurely to an HIV-positive mother, the babies died shortly after birth. So although he is fluent in the language, the tireless doctor chose not to tell Mufuka that her unborn babies were unique and uniquely fragile. He opted for a few honest details – saying simply that she was carrying mapatya (twins), they would be delivered by Caesarean section, and may not survive. A man of faith, Dr. Thistle then banked on chishamiso – a miracle.
Two weeks after Mufuka’s first ultrasound, Dr. Rachel Spitzer, an obstetrics and gynecology resident at the University of Toronto, arrived at Howard Hospital. In 2003, Dr. Spitzer had done several days of clinical work at the Howard, and now she was back for a three-month clinical and research residency involving HIV transmission from expectant mothers to their babies. She was also keen to assist Dr. Thistle with his patients. The two doctors had an easy connection. And it wasn’t long before their simpatico working style would be tested by a once-in-a-lifetime birth.
On July 20, a few hours before one of the region’s blazing sunsets, Mufuka showed up for her weekly appointment appearing uncomfortable yet typically stoic. “We examined her and she was without question in labour,” recalls Dr. Spitzer.
Dr. Thistle gathered his staff in the operating room and informed them the twins were set to arrive. He would assist Dr. Spitzer with the C-section. “There was the nervous expectation that these kids were going to survive,” says Dr. Thistle, adding that there was also the unspoken question of “What next?” Ten minutes later, the twin boys were lifted from their mother’s womb without incident, much to the relief of the doctors who were amazed at what they had done. “They came out screaming,” says Dr. Spitzer. “It was an easy delivery.”
Tinashe and Tinotenda were swaddled and then fell asleep contentedly in the maternity ward. Meanwhile, the question of “What next?” weighed heavily on the two Canadians who had brought the boys into the world. It wasn’t long before Drs. Thistle and Spitzer began looking homeward to Toronto for an answer.
***
Conjoined twins are a kind of miracle of incomplete separation. As with identical twins, they form when an ovum splits into equal halves during early embryonic development. The difference is they fail to completely cleave from each other during the crucial first two weeks. The resulting fusion of two bodies has its own unique variations. Conjoined twins often share a major organ such as a brain, heart, liver or bowels. They always share skin and only sometimes bones, genitalia and entire limbs. And they are rare – as few as one in every 50,000 to 200,000 pregnancies. Science has yet to divine why they occur, and nature has largely not been on the side of their survival. Half of conjoined twins are stillborn; one in three live for only a few days.
Surgical attempts to remedy nature’s unfinished work in creating two individuals began as early as the 1600s. But it wasn’t until the 1950s that a few leading pediatric hospitals around the world began devoting resources to helping these unique children. A conflux of medical advances made separation surgeries more viable – particularly the huge leap in diagnostics that occurred with the development of MRIs and CAT scans, which allow doctors to see exactly how and where conjoined twins are fused. But separation surgeries are still the province of the largest, best hospitals in the world – institutions with a critical mass of money, equipment, multidisciplinary expertise and, typically, a university affiliation.
“The teaching hospitals are our university and the university is the hospitals,” says Dr. Richard Reznick, chair of U of T’s surgery department in the Faculty of Medicine. “As a research-intensive university our business is high-end surgery and the complex cases that others aren’t positioned to do.”
In 1966, the first surgical separation of conjoined twins in Canada was attempted at The Hospital for Sick Children, a U of T teaching hospital. But it wasn’t until two decades later that the institution gained international prestige for its expertise in the surgery. That’s when Lin and Win Htut, Burmese twins joined laterally at the pelvis who had been languishing in a Rangoon hospital because doctors there didn’t know what to do with them, came to the attention of Dr. Robert Filler, then surgeon-in-chief and chief of general surgery at Sick Kids.
There is nothing routine about surgically separating conjoined twins. “It’s not like you get a 1,000 of these done this way and 1,000 done that way and then you compare the outcomes and make a decision,” says Dr. Filler. “The numbers are too small.” The cases are so rare that a doctor must bring to the surgery a full career’s worth of understanding – an advanced knowledge of physiology, anatomy and surgical principles and experience with complex surgeries such as organ transplants. Clinical experience is paramount.
Dr. Filler had helped surgically separate twins in the United States, and he convinced the hospital’s Herbie Fund, an international charitable organization that provides children with treatments not available in their home country, to help finance the Htut twins’ surgery and care. In 1984, amidst a flurry of media attention, the Htuts were successfully separated at Sick Kids. More cases would follow. Today, a total of 10 separation surgeries have been performed at the Toronto institution.
“[At the time], there was very little written in the medical literature about conjoined twins,” says Dr. Filler. “I thought it was wisest to have experts in each of the specialties involved, so I put together very large teams.”
One of those early team members was Dr. Ron Zuker, a plastic surgeon and now also a professor at U of T. He had collaborated with Dr. Filler on how to cover the large wounds left by separation surgeries using tissue expanders, a technique already employed in other plastic surgery. In this procedure, silicone balloons are inserted under the skin near the future wound area and then gradually filled with salt water so the skin stretches and grows around them. In 1985, Drs. Filler and Zuker were the first surgeons to adapt tissue expanders to separation surgery when they flew to Trinidad and inserted expanders in the abdominal cavity of conjoined twins Heera and Shiva Ramkhalawan, several months before they were scheduled for separation at Sick Kids.
Dr. Filler’s collaborations and “big-team” approach allowed knowledge of these rare cases to radiate to all who participated. As a young pediatric surgeon, Dr. Jacob Langer assisted in two separation surgeries with Dr. Filler. (As head of general surgery, he later participated in a third separation.) Then in 1999, Dr. Langer followed in Dr. Filler’s footsteps by being appointed Sick Kid’s chief of general surgery.
“There is no specific collaboration between the university and the hospital that makes complex surgery more possible,” says Dr. Langer who is also a U of T surgery professor. “However, it is the relationship between the university and the hospital that creates the environment of academic excellence and attracts the most creative and talented minds to come here, both to train and to work. It is because we can build multi-disciplinary teams out of those kinds of people that we can take care of such complex surgical patients, who are referred to us from our own community and from around the world.”
***
Dr. Langer’s name was being whispered in hopeful breaths within 24 hours of Tinashe’s and Tinotenda’s noisy, remarkable debut at Howard Hospital.
Other international hospitals responded to Drs. Thistle’s and Spitzer’s inquiries but they lacked charitable support. When Dr. Langer replied he was interested in the case and copied his response to the director of the international patient office at Sick Kids that oversees the Herbie Fund, Drs. Spitzer and Thistle hoped they were closing in on the “great Canadian effort” for which they’d secretly been rooting.
But Dr. Langer needed more information to make his case to the Herbie Fund. “You can imagine how complex the whole process of human development is,” he says. Well, that’s how complex the process of separating twins is.”
At Howard Hospital, phones are unreliable and sending and receiving e-mail means a 60-minute drive to Harare. Even there, the technology is archaic by Western standards. “There is no high-speed internet in Zimbabwe. Period,” says Dr. Spitzer.
Three weeks after the twins were born, she taped an X-ray of the babies to a well-lit Howard Hospital window and snapped a picture of it with her digital camera. Using a slow Internet connection in Harare, it took her several hours to e-mail the image and a few other digital photos to Dr. Langer. But it paid off.
The images confirmed that Tinashe and Tinotenda were omphalopagus conjoined twins – attached abdominally at the liver. And it was also evident that each baby had all the organs a person needs to survive. But without the surgery they would likely meet a premature death.
Within two months of the twins’ birth, there were solid plans to bring the babies to The Hospital for Sick Children where they would be evaluated for a $200,000 separation surgery.
“Blest be the ties that bind,” says Dr. Thistle. “I’ve worked as a medical student and resident at Sick Kids. It was like a homecoming.”
***
By the end of September, Dr. Spitzer’s three-month rotation in Zimbabwe was over. The twins, then two months old, were not growing well, their feeding inhibited by their cleft lips and palates and the Howard’s limited resources. “I was sad to be leaving them,” she says. “But I also knew the best way to get them over here was to come back and start working on it more.”
So when Dr. Spitzer hit the ground in Toronto she became a fundraising fanatic – firming up already-committed donations and finding others for expenses the Herbie Fund could not cover. Ve’ahavta, a Canadian Jewish humanitarian organization, offered social support and accommodation. The Salvation Army of Canada covered the $5,000 plane tickets. And many individuals – from those at Dr. Spitzer’s synagogue to the engineering firm where her father works – made personal donations.
Dr. Spitzer did not have to wait long before seeing the twins again. On Dec. 2, she drove to Pearson International Airport to pick up Mufuka, the twins and a nurse midwife named Grace who would act as a translator. On landing from their 18-hour flight from Harare, the Zimbabweans looked out the plane window and saw snow for the first time in their lives – the beginning of many strange new zvishamiso (miracles) Toronto would offer.
***
To orchestrate a separation surgery you need a physician with specialist training and also a generalist’s knack for understanding all the variables at play – a lead violinist who is an adept conductor. Dr. Langer had experience on his side, and he enlisted the help of Dr. Zuker, himself a veteran of seven separation surgeries. Other specialists eagerly offered their services for free. Soon, the team had expanded to include two general surgeons, two plastic surgeons, two anesthetists and an assortment of medical residents and eight nurses – 25 professionals in total.
Tinashe and Tinotenda were malnourished when they arrived in Toronto. But by March 2005, with more specialized medical care, they were robust and ready for surgery. There was a glitch in the plans, though. The tissue expander that Dr. Zuker had inserted over the shared part of the twins’ abdomen and lower chest, the area they were most worried about having enough skin to cover, had become infected. All the new skin was lost – a big blow, given wound coverage is one of this surgery’s biggest challenges. New techniques were required.
Dr. Langer has written 175 papers for peer-reviewed journals and 34 book chapters, and among his areas of expertise is repairing abdominal defects in children. In these cases, he often uses surgical mesh to strengthen and close the abdomen. But older materials, such as Gore-Tex, don’t dissolve in the body and neither do they grow with a developing child. Recently, Dr. Langer had tried a new support material called Surgisis, bioengineered from pig cells, that’s strong and can be absorbed by the body. “The patient’s own cells grow into this patch so the patch ends up dissolving and is replaced by the patient’s scar tissue,” explains Dr. Langer. He decided to use Surgisis for Tinotenda, the smaller twin, who would have the larger wound and need support for his abdomen and chest walls.
The other tricky variable was the amount of anesthetic to give each child. The twins shared a blood vessel in the liver, which shunted more blood and nutrients to Tinashe. There was no way to know how much each twin weighed separately and how much of one baby’s anesthetic would end up in the blood supply of the other. “We risked giving an overdose to one and an inadequate amount to the other,” says Dr. Cengiz Karsli, the lead anesthetist for the surgery. In the end, they treated the twins as if they were of equal weight. Dividing the boys’ livers was less of a worry, says Dr. Langer. Although the livers joined over a large area, they were actually separate organs, each with its own bile drainage and blood supply.
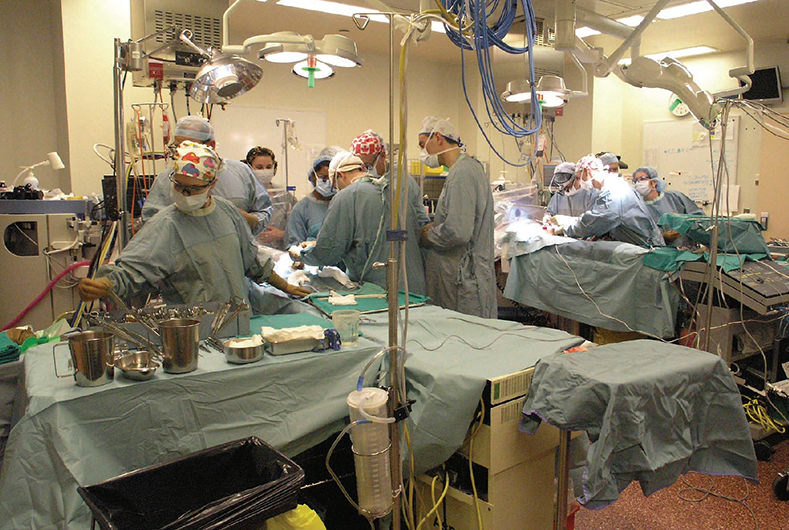
At 9:33 a.m. on Mar. 7, Dr. Langer and his team began the painstaking work of separating the twins. A little more than five hours later, Tinashe and Tinotenda were recovering in the critical care unit – in separate beds for the first time in their lives.
***
Dr. Thistle often encourages his patients with the saying Kugarika tange nhamo, rugare rugotever, or “What is sown with tears will be reaped in laughter.”
On a promising afternoon in early April – just shy of a month after their surgery – a beaming Elizabeth Mufuka displayed her two separate sons, Tinashe and Tinotenda, newly released from the hospital, to an ogling klatch of media.
The twins will stay in Toronto for another few months to have their cleft lips and palates repaired. In June, Paul Thistle plans to bring his family to Toronto for a vacation. If all works out as hoped, he will visit the newly separated twins in the bosom of Canadian health care before they return home to Zimbabwe and its sparer health-care realities.
The Canadians whose lives have intersected with the twins – from Drs. Thistle and Spitzer, to University of Toronto senior surgeons Drs. Langer and Zuker, to the many in the community who supported them – use words like “surreal,” “extraordinary” and “fascinating” to describe the medical challenges and humbling human encounters that, for a short time, joined their lives with a very distant place. “You realize what you can achieve … as an individual and as a community,” says Dr. Spitzer. “The world’s not such a big place sometimes.”
In Shona, they might say Zvishamiso zvakawanda zvauya – “Miracles many came.”
Krista Foss is a freelance writer in Hamilton, Ontario.
Recent Posts
People Worry That AI Will Replace Workers. But It Could Make Some More Productive
These scholars say artificial intelligence could help reduce income inequality
A Sentinel for Global Health
AI is promising a better – and faster – way to monitor the world for emerging medical threats
The Age of Deception
AI is generating a disinformation arms race. The window to stop it may be closing